Were you or a loved one misdiagnosed with skin cancer? We understand the anger, frustration and fear you must be facing.
- How will we pay for our medical expenses?
- Who can be held liable for my injuries?
- Can we pursue financial compensation?
Affected by a cancer misdiagnosis? Our experienced medical malpractice attorneys can help. Learn more in a free consultation.

(877) 996-5837
When medical professionals make critical errors, our experienced legal team is here to help patients pursue justice.
Taken as a group of disparate diseases, skin cancer is likely the most common form of malignancy affecting patients in the United States. Over 3.3 million Americans are diagnosed with some type of skin cancer ever year, the American Cancer Society says. But it would be a mistake to think of skin cancer as a single thing. In reality, researchers have defined multiple types of skin cancer, all of which behave differently, progress on average at faster or slower rates and present themselves with separate symptoms.
Understanding Skin Cancer & Medical Negligence
Before we start about what distinguishes these cancers from each other, let’s talk about what makes them similar. Like all forms of cancer, skin cancer is fundamentally a genetic disease, one caused by mutations in the DNA of once-normal cells. And the vast majority of skin cancers are the result specifically of genetic mutations caused by exposure to ultraviolet radiation, the Skin Cancer Foundation says, either from the sun or tanning beds.
The diagnostic protocol is also similar. While symptoms are certainly a clue to cancer, oncologists universally believe that the only way to truly diagnose skin cancer is through a biopsy.
FREE CONSULTATION
Basal Cell Carcinoma
The most common form of skin cancer is called basal cell carcinoma, or BCC, because it starts near the bottom (or “basal”) layer of skin cells. Around 800,000 people in the US are diagnosed on a yearly basis, often after noticing a new growth on their skin, usually the head, neck or arms. Technically, this growth isn’t a mole, although it can sometimes look like a mole.
Moles are created by melanocytes, cells that manufacture the pigment (melanin) that gives our skin color. And most moles aren’t cancer. The bumps associated with basal cell carcinoma, on the other hand, are actually cancerous tumors. In most cases, these growths will appear pink, brown or black, but will often be traced inside by blood vessels, according to WebMD. It can look like a pimple, but a pimple that doesn’t go away after a few weeks. Sometimes, the surface of the growth will feel scaly to the touch, but BCC tumors can also be waxy or hard.
Misdiagnosing BCC
Most cases of basal cell carcinoma are diagnosed properly and treated in a timely fashion, but due to the disease’s appearance, some patients are misdiagnosed and told they have acne, according to recent research in Clinical Case Reports. Acne, however, usually responds to treatment, either using topical creams, oral pills or laser therapy. Skin cancer doesn’t, so when a growth that looks like a pimple fails to respond to these therapies, physicians should begin to suspect BCC.
Unlike most types of cancer, basal cell carcinoma doesn’t usually spread (or metastasize) to distant organs. BCC usually stays in the skin. The biggest risk, as the American Academy of Dermatologists notes, is that the cancerous cells will move a little deeper, invading nearby bones or body tissues. That can lead to tissue damage and physical disfigurement. Thankfully, basal cell carcinoma is very treatable, when it’s caught at an early stage, since BCC tends to grow slowly.
Squamous Cell Carcinoma
The second most common form of skin cancer is called squamous cell carcinoma, or SCC. These malignancies develop in squamous cells, which form the outer surface of the skin. Around 660,000 people in the United States are diagnosed with the disease every year, most of whom are in their 60s or 70s.
What Is Bowen’s Disease?
At it’s earliest stages, SCC is often referred to as Bowen’s disease. Bowen’s disease is characterized by a scaly patch of red skin, either flat or raised. The discoloration can look like an odd sort of red bruise, but one that doesn’t heal. In most cases, this first sign of Bowen’s disease feels scaly or crusty to the touch, like a sore or gradually-healing scab. It’s not always itchy, Britain’s Natural Health Service says, but it can be.
While Bowen’s disease is technically a form of cancer, it’s far from dangerous when diagnosed promptly. Dermatologists have a range of ways to deal with the condition, all of which are remarkably effective. The patch of abnormal cells can be frozen off, scraped away or eliminated through the use of lasers.
Cancer Progression & Complications
When Bowen’s disease goes undiagnosed, it can get worse, burrowing further below the skin’s surface to become squamous cell carcinoma. This transition is often accompanied by a change in symptoms. The patch of red skin that began as Bowen’s disease can crack open, turning into an ulcer, bleed or grow into a larger lump. These are all signs that the skin cancer may be progressing.
Overtime, an undiagnosed case of squamous cell carcinoma can lead to extensive tissue damage, even the loss of an entire organ, like the nose or ear. Despite the progression in severity, most cases of SCC are treated in the same way as early cases of Bowen’s disease, by removing the malignant cells through surgical means, freezing or topical creams.
How Do Doctors Misdiagnose SCC?
Again, severe complications from SCC are uncommon, since most cases are diagnosed when the cancer is still classified as Bowen’s disease. But we should note that the early signs of Bowen’s disease can appear very similar to other skin conditions, including psoriasis or eczema. These superficial similarities can trap some physicians into making the wrong diagnosis, dismissing a malignancy as the result of some more-common, but far less-dangerous, disorder.
Malignant Melanoma
Melanoma is the least common form of skin cancer, but also the most aggressive. In 2017, over 95,000 new cases of skin cancer were diagnosed in the United States, according to the American Cancer Society. More than 87,000 of these cancers were classified as melanoma.
So what, exactly, is this disease that strikes nearly 100,000 Americans every year? Like all forms of skin cancer, melanoma is defined by the sort of cell where it begins. The cancer starts, according to the Melanoma Research Foundation, in melanocytes, cells that create melanin, the pigment that colors our skin, eyes and hair. While melanocytes aren’t exclusive to the skin, most can be found there, which is why most cases of melanoma are ultimately defined as “cutaneous,” relating to or affecting the skin.
Alongside the skin, melanocytes can also be found in the mucus membranes of our body, as well as the eye’s iris (the part with color). Though extremely rare, some forms of melanoma can be found in the mucus membranes (usually the sinuses, nasal passages or mouth) or eye.
Melanoma Symptoms & Signs
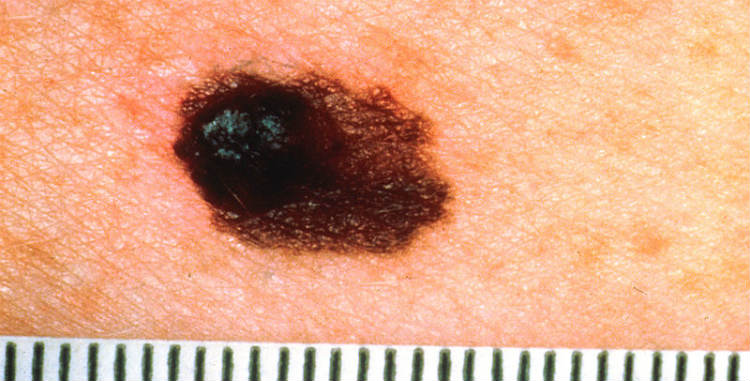
This cancer should be easier to diagnose than other forms of malignancy. Since most cases of the disease develop on the skin, the initial signs of the disease are, in theory, visible to the eye. In their early stages, melanoma tumors often look just like normal moles. And around 30% of melanoma cases begin as existing moles, according to researchers in the Journal of the American Academy of Dermatology.
This is an odd situation in the world of cancer. Of course, most moles will never become malignant. But those skin cells that do become cancerous often originate in moles. Other cancers don’t work like this. The vast majority of cancers, beginning somewhere inside the body, only lead to “non-specific” symptoms at first. When we say “non-specific,” we mean that the symptoms could be caused by any number of less-severe medical conditions. So it’s easy to confuse a diagnosis, even for the best cancer specialists.
Changes In Moles: What To Watch Out For
The signs of melanoma, on the other hand, should be a little more apparent. Alongside the development of new moles, you should watch for odd changes in the skin, the Mayo Clinic reports:
- Changes In Existing Moles – Normal moles are usually a single color, fairly-small and separated from the surrounding skin by a distinct border. Cancerous or pre-cancerous moles, on the other hand, can appear:
- asymmetrical – mole looks lopsided
- border – mole has an irregular border with notches
- color – mole is multicolored
- diameter – existing mole grows larger than 1/4 inch in diameter
- evolving – mole’s appearance changes over time
- Other Changes In Moles – While the ABCDE mnemonic is helpful, some changes in moles should be cause for concern, but don’t fit in:
- Pigment spread – watch for places where the color of a mole begins to spread to surrounding areas of skin
- Redness and inflammation – look for signs of irritation around an existing mole
- Surface texture – pre-cancerous moles can become scaly, or may bleed
- Symptoms Other Than Moles – Some cases of melanoma don’t fit into the picture that begins and ends with moles. Watch for skin sores that fail to heal, along with areas of skin that suddenly become more tender or itchy.
Be especially careful to watch for symptoms and signs on parts of your skin that are often exposed to the sun, like your back, arms, face or the top of your head if you’re losing your hair. People with darker skin tones should also be careful to check places that don’t get a lot of sun exposure, including the soles of your feet and the palms of your hands.
Why Does Cancer Happen?
In essence, cancer begins when cells lose the ability to die, as our healthy cells do on a normal basis. Normal human cells commit suicide for two basic reasons:
- intrinsic apoptosis – a cell, of its own accord, recognizes that some form of stress (heat, viral infection, lack of oxygen or DNA breakdown, for example) has made living further untenable
- extrinsic apoptosis – other cells “tell” a cell to die, normally because it’s been pegged by the immune system as infected or abnormal
In either case, the cells begins a chemical process, known as apoptosis, that eventually rips it apart. Around 50 to 70 billion cells die every day in the average human body, for perfectly normal reasons. Cancer is the word we use to mark cells that have lost the ability to die. Normally, this change is the result of genetic mutations. An errant quirk of DNA allows the cell to ignore external signals that would trigger apoptosis, or disregard internal signs of degradation.
Instead of committing suicide, the cell just divides and divides and divides, passing the cancerous mutation on to its progeny. Most cancer cells also gain the ability to cloak themselves from immune system cells, which prevents them from being eliminated by the body’s defenses. This is the basic problem of cancer. Malignant cells divide uncontrollably, forming tumorous masses, crowding out healthy cells, colonizing normal body tissues and, in the case of metastatic diseases, spreading far from their site of origin.
Who Gets Skin Cancer?
White people are far more likely to develop skin cancer, dermatologists write in the journal Cancer Control, but some forms of the condition, including melanoma, are more likely to spread in black and Latino people. In short, everyone should be concerned about getting skin cancer, regardless of your skin color. With that being said, people who sunburn easily (especially when the skin blisters) live at the highest risk of developing the disease.
How Should Doctors Diagnose Skin Cancer?
Most dermatologists get a clue to the presence of skin cancer after noting a suspicious new skin growth or hearing from a patient about odd changes in their skin’s appearance. That’s why health experts recommend receiving an annual skin exam from your doctor, because the initial signs of skin cancer are often apparent to the eye, through a simple non-invasive evaluation. After reviewing your symptoms, the doctor is also likely to investigate your personal history. Questions about tanning and sunburns are common, the MD Anderson Cancer Center reports, since ultraviolet light exposure is the leading risk factor for all forms of skin cancer.
Skin cancers rarely kill people. As we’ve seen, something like 3.3 million Americans are diagnosed with a skin cancer every year. Only around 2,000 people will die from the diseases during the same period, according to the American Cancer Society. Even so, receiving a misdiagnosis can impact a patient’s life in disastrous ways, to say nothing of the lives of their family and loved ones.
Learn More About Filing A Skin Cancer Misdiagnosis Lawsuit
In some cases, patients may be eligible to secure financial compensation in the wake of a cancer misdiagnosis. If a doctor, nurse or radiologist provided you with sub-standard care, you may be able to hold them accountable by filing a medical malpractice lawsuit, pursuing damages to compensate for the harm that the misdiagnosis has caused.
To learn more about your legal rights, contact the experienced malpractice lawyers at Monheit Law for a free consultation. Our attorneys can help you gain perspective on your various options and discuss the possible steps forward. If we can help in your case, we’ll offer our legal services on a contingency-fee basis. That means you owe our lawyers nothing until we secure compensation for you and your loved ones. Find more information today by calling our attorneys or completing our online contact form.
Monheit Law Montgomery County Office 215-866-2018
Directions to our Montgomery County Injury Law Office
4V4Q+FM Jenkintown, Pennsylvania
Open 24 hours
Skin cancer misdiagnosis attorney Jenkintown
Civil law attorney
Employment attorney
Law firm
Attorney
Social security attorney
Monheit Law South Philly Office 215-302-0095
Directions to our South Philly Injury Law Office
WRCH+CP Philadelphia, Pennsylvania
Open 24 hours
Skin cancer misdiagnosis attorney South Philly
Civil law attorney
Employment attorney
Law firm
Attorney
Social security attorney
