Informed consent is a critical medical principle. All patients have a basic right to understand the complications and risks of the medical procedures they undergo.
- Were you or a loved one misled about the risks of a medical procedure?
- Did you suffer severe injuries?
- Financial compensation may be available
Our experienced medical malpractice attorneys can help. Find more information in a free consultation.

(877) 996-5837
Every patient has a fundamental right to understand the risks and complications of medical procedures.
As a medical patient, you have the right to make personal decisions about your health. In both moral and legal terms, you are an autonomous agent – entitled to make decisions on your own behalf free from interference. Informed consent laws, passed and enforced by state governments, are designed to protect this concept of patient autonomy and allow patients to make the best decisions for their future.
Medical Consent Laws In Pennsylvania
In Pennsylvania, doctors suggest the treatments they think would work best for a patient. Patients, on the other hand, choose to undergo diagnostic tests and procedures. To meet legal and ethical standards, state laws agree that patients must give their voluntary informed consent to most forms of medical treatment, including diagnostic tests and procedures.
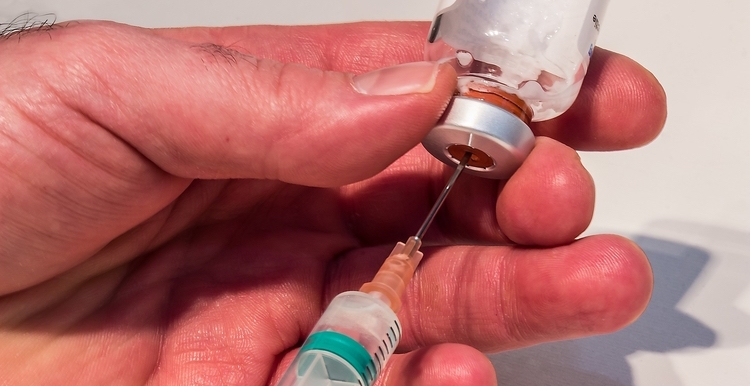
The vast majority of state-level informed consent laws recognize that educating a patient fully is a formal precondition for consent. To comply with this requirement, physicians must adequately inform patients of the benefits and risks of a medical procedure, along with alternative treatment options. When doctors fail to uphold this obligation, and patients develop an undisclosed risk or side effect, the affected individuals may be able to secure financial compensation.
FREE CONSULTATION
The Basics Of Informed Consent
Consent, in the modern world, requires both ability and freedom.
To make the best decision about their own care, patients must be able to make the decision. In this context, ability is a function of information and understanding. You can’t truly consent to a treatment if you don’t know anything about it. That’s why medical professionals refer to informed consent, rather than consent alone. The only way to consent freely to a treatment is through adequate information. Likewise, you can’t truly use the information presented until you actually understand it. Informing is something that doctors do, but understanding is something that patients do. As a result, informed consent implies two corresponding duties:
- physicians must inform their patients of benefits, risks and alternatives
- patients must ask for clarification when they don’t understand the presented information
Informed consent always entails freedom of choice. It must be voluntary. You can’t feel pressured or coerced into taking a drug or undergoing surgery. Your consent to treatment is a choice that you make because you believe, truly believe, that the treatment is a good option for you.
Speak Up In Medical Consultations
A doctor’s disclosure must be communicated in language that the patient can understand. Highly-technical terms should be avoided or, alternatively, explained clearly. A patient’s primary language should also be taken into account. When English isn’t the patient’s first language, a translator may be required.
Like any process of education, informed consent shifts certain obligations to the “student.” Patients should speak up when a detail doesn’t make sense. In most cases, doctors will assume that, when patients don’t ask for clarification, they understand the procedure or drug. Mind-reading is not in the normal physician’s toolbox.
Two Legal Theories Of Doctor Disclosure
What constitutes adequate disclosure? States take one of two avenues on this question. Most states, according to Bryan Liang, MD, a professor of healthcare law at the University of Houston, use a provider-centered standard – doctors should give their patients all the information that a reasonable healthcare professional would provide under similar circumstances.

A minority of states, including Pennsylvania, use a patient-centered standard – doctors should give their patients all the information that a reasonable patient would require to make an informed treatment decision. Again, this is the standard considered in Pennsylvania’s courts.
Necessary Information
While each standard is shaped by its own nuances, both provider-centered and patient-centered disclosure require physicians to cover the same basic categories of information before a treatment can be started:
- the patient’s diagnosis
- the goal of treatment and probability of success
- the risks posed by treatment
- alternatives to the proposed treatment, even when the doctor feels that these alternatives would be inappropriate (poorly-substantiated “alternative” treatments need not be covered)
- the risks and benefits of refusing treatment
There are some facts that doctors don’t usually have to disclose, even though they are true. Obvious, common-sense risks, ones that would be apparent to a reasonable patient without special guidance, are one example. Doctors aren’t usually required to disclose each and every potential risk, either; extremely-rare side effects, for example, can usually be left out. The same goes for risks that a competent doctor would not have been able to foresee.
When Is A Patient’s Sign-Off Required?
State laws define two broad forms of consent:
- implied consent
- express, or written, consent
While the purpose of every exam or procedure should be explained beforehand, a patient’s consent can, in some cases, be implied by their actions. A patient who rolls up her sleeve for a blood pressure cuff, for example, is usually taken to have consented to the exam, whether or not she signs a form. Implied consent is generally accepted for routine and basic examinations, including annual physical exams with your doctor.
Signing A Consent Document
Invasive procedures are another story. When an exam or procedure carries significant risks, or there are suitable alternatives to consider, state laws require express consent. Patients have to formally consent to serious procedures beforehand, usually by signing a consent document and accepting the potential risks and rewards of a chosen treatment.
Note, however, that signing a consent form isn’t the same as actually giving your informed consent. Signed consent documents simply show that you believed you had been fully-informed. As a patient, it’s not your duty to know, before the fact, which medical details will be crucial to your treatment decisions. Those details are selected and communicated by a medical professional.
Which Procedures Are Covered By Pennsylvania Law?
The legal principles behind informed consent have been recognized in Pennsylvania’s common law tradition since at least 1932, according to Physicians News Digest. That year, the State’s Superior Court affirmed that patients have the right to consult with their physicians about treatment options. Patient consent, the Court wrote, is an essential precondition of medical treatment. Thirty-one years later, in 1963, the Pennsylvania Supreme Court formally adopted this rule, shaping the way state courts would view informed consent for decades.
Until fairly recently, however, Pennsylvania state law only required informed consent before surgical procedures. The Health Care Services Malpractice Act, a law passed in 1997, changed that, expanding the number of situations in which express consent is mandatory. Today, express informed consent is required before the following treatments are performed:
- surgical procedures
- the administration of anesthesia during surgery
- chemotherapy and radiation therapy
- blood transfusions
- implantation of surgical devices or appliances
- experimental medications and medical devices
- use of an approved medication for an experimental purpose
At the moment, Pennsylvania law does not require informed consent prior to the administration of antibiotics, non-experimental medications or orally-administered prescription drugs. Most treatments performed by chiropractors, including chiropractic manipulations, are not covered by the State’s informed consent laws.
Who Must Secure Consent?
In Pennsylvania, physicians must take personal responsibility for acquiring informed consent from their patients. According to a 2017 opinion of the State’s Supreme Court, doctors, and only doctors, have a legal obligation to secure informed consent. In the Court’s decision for Shinal v. Thomas, a case involving a botched brain surgery, Pennsylvania Supreme Court Justice David Wecht wrote,
“Without direct dialogue and a two-way exchange between the physician and patient, the physician cannot be confident that the patient comprehends the risks, benefits, likelihood of success and alternatives. Only by personally satisfying the duty of disclosure, may the physician ensure that consent truly is informed.”
This duty, Law360 reports, cannot be delegated to subordinates, including resident physicians or nurses. Thus, only physicians can be held accountable for failing to secure a patient’s informed consent.
No “Vicarious Liability,” PA Supreme Court Rules
This distinction alone places informed consent violations at odds with most medical malpractice cases. In many malpractice claims, hospitals can be held at least partially liable for an employee’s mistakes, via a legal doctrine known as “vicarious liability.” However, Pennsylvania state court precedent holds that vicarious liability does not apply in cases related to informed consent.
Major Exceptions
State laws generally recognize two major exceptions to the concept of informed consent:
- emergency medical care
- diminished patient autonomy
When immediate medical care is required to prevent severe or irreparable patient harm, informed consent isn’t usually required. Delays in emergency care can have permanent consequences; as a result, most states provide doctors with legal wiggle room when the process of securing informed consent would prevent a life-saving treatment from being administered in time.

That doesn’t mean that informed consent disappears in the emergency room. The general standard applied in emergency medical treatment is that informed consent should be obtained for conscious patients who are not prevented from making logical decisions by an emergent medical condition. In emergency circumstances, however, informed consent may not be required.
Minors & Legally Incompetent Adults
State laws recognize that the rights of patients with “diminished autonomy,” like children and adults with cognitive disabilities, should be protected. Some people, due to their age or mental capacity, are considered unable to consent or refuse medical treatment. In these cases, the right to provide informed consent is transferred to parents or legal guardians. Informed consent is still required, but it might not come from the patient. However, there are major exceptions to this general rule. Pennsylvania law allows some minors (usually children over the age of 14) to consent, without the intervention of parents or legal guardians, to specific forms of medical treatment. To learn more about these exceptions, visit our Informed Consent FAQ.
The Structure Of An Informed Consent Lawsuit
What happens when a doctor performs a diagnostic test or medical procedure without securing informed consent? In some cases, patients who ultimately suffer side effects or complications that were not properly disclosed will be able to file a civil lawsuit against their physician. This is not, however, a claim for medical malpractice. In Pennsylvania, failing to acquire informed consent is considered a form of battery:
- Battery – the intentional touching of someone else in an offensive or injury-causing manner
Negligence doesn’t come into the equation. It does not matter, in the context of an informed consent claim, whether or not the doctor made a careless mistake in administering medical care. The crucial point is simply that the doctor administered medical care to which the patient did not provide their informed consent.
Also irrelevant is whether or not a reasonable patient, having been properly informed of a procedure’s risks and alternative options, would have consented to the treatment. In Pennsylvania, patients have an absolute right to “medical self-determination,” including a right to make unreasonable choices about their care.
As a result, patients have no obligation to prove that they would have made a different choice based on more accurate information. The standard is minimal; patients need only demonstrate that the medical information not provided to them would have been a “substantial” (or “material”) factor in their decision-making process.
Strict Time Limits Apply
Pennsylvania has a variety of laws, collectively known as the “statutes of limitations,” that restrict the amount of time injured people have to file civil lawsuits. In most cases, claims against medical professionals, including professionals, must be filed within two years.
The time period begins, however, according to a “discovery rule,” which holds that injured patients should be given adequate time to discover the connection between their injuries and a medical error or procedure. In other words, most patients who plan to file suit will have two years from the day they learn (or should have learned) that a doctor’s actions may have caused their injuries. Another law, the “statute of repose,” serves as a hard deadline. No lawsuit can be filed against a medical professional in Pennsylvania more than seven years after harmful conduct took place.
Wrongful death lawsuits are a notable exception. When a decedent’s estate chooses to file suit, the estate has two years beginning on the date of death.
Different Deadlines For Minor Victims
Another exception to this general two-year time frame is usually applied when the person who suffered an injury is a minor – under the age of 18. Children are normally given two years, beginning on the day they turn 18, to file a civil lawsuit. The statute of repose is also different for child victims. Minors lose their right to file suit either seven years after the alleged wrongdoing or upon their 20th birthday, whichever date is later.
Monheit Law Montgomery County Office 215-866-2018
Directions to our Montgomery County Injury Law Office
4V4Q+FM Jenkintown, Pennsylvania
Open 24 hours
Medical consent attorney Jenkintown
Civil law attorney
Employment attorney
Law firm
Attorney
Social security attorney
Monheit Law South Philly Office 215-302-0095
Directions to our South Philly Injury Law Office
WRCH+CP Philadelphia, Pennsylvania
Open 24 hours
Medical consent attorney South Philly
Civil law attorney
Employment attorney
Law firm
Attorney
Social security attorney
