The US Department of Veterans Affairs is protecting bad doctors, according to a series of new reports from USA Today. Despite its mission to care for America’s veterans, the VA has hired dozens of physicians with lengthy malpractice records and license suspensions, doctors who often go on to hurt VA patients. When problems arise, USA Today finds, the federal agency has a habit of concealing the misdeeds of physicians from the public, allowing dangerous healthcare professionals to transition smoothly into private practice.
VA Faces Medical Malpractice Scandal
A USA Today investigation published on December 3, 2017 focuses on Dr. John Henry Schneider, a neurosurgeon whose allegedly substandard care led to over 12 medical malpractice cases in Montana and Wyoming, the two states in which he practiced prior to 2017. “That’s certainly not normal,” says Larry Schlachter, a neurosurgeon and medical malpractice attorney. Racking up 12 medical malpractice in 12 years, the expert told reporters, definitely makes Schneider an “outlier.”
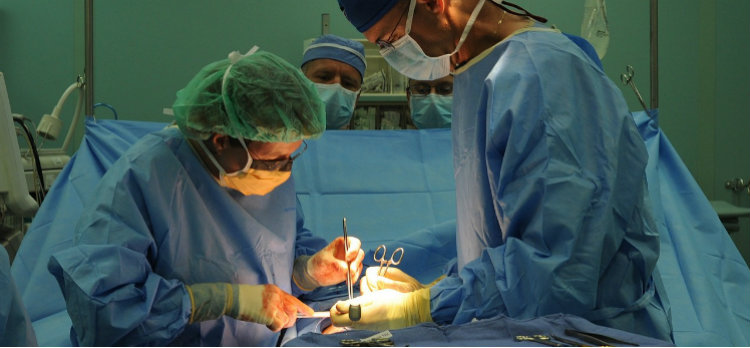
After one of Schneider’s surgical patients died of complications, the State of Wyoming’s Board of Medicine revoked the physician’s medical license. And, buried in medical malpractice claims, Schneider applied for bankruptcy in 2014, telling a Montana Court he had amassed a personal fortune of $17 million but had “virtually no assets.” Per an eventual bankruptcy settlement, Schneider’s former patients secured $0.15 on the dollar for their $7 million in claimed damages.
Federal Hospital Hired “Dangerous” Surgeon
Then, in the early months of 2017, Schneider applied to work at the Veterans Administration hospital in Iowa City, Iowa. He was, as USA Today writes, “forthright” in his application about the past, explaining to federal regulators that he had been sued for medical negligence on numerous occasion and Wyoming had stripped him of his license. Despite his controversial history, Schneider was hired by VA and began working at the Iowa City hospital in April. His starting salary? $385,000 per year.
It wasn’t long before patient complications began to surface. A 77-year-old veteran named James Wehmeyer was left with a severe infection after Dr. Schneider conducted a spine surgery on him in July. Wehmeyer underwent two subsequent procedures, all performed by Schneider, to fix the problem. Schneider denies all wrongdoing. “I’ve had a great run at the VA with zero issues,” the doctor told USA Today. “Have I had to take patients back for post-op infection? Yes. I mean, I can’t prevent every infection.”
Schneider’s accusers were shocked to learn of his hiring by the VA. “How does this happen, especially with a neurosurgeon?” asked Sherry Lee. In 2012, Lee underwent a neck surgery in Wyoming. Dr. Schneider was at the helm of the operation, which was an utter failure, the patient says. Lee was left with severe pain and functional impairments, her subsequent lawsuit claims. Now that Schneider’s money is being managed by a bankruptcy court, the woman is still waiting for her share of the payout.
Fired From VA, Arrested By Federal Officials
The real kicker, however, came in September 2017, when federal prosecutors filed criminal charges against Schneider, saying the neurosurgeon had lied about his assets during bankruptcy proceedings. He was arrested in Southern California on five counts of bankruptcy fraud, the Billings Gazette reports. VA officials have now determined that Schneider’s hiring was illegal, since federal law prevents the agency from employing any doctors who have had their State medical licenses suspended.
Do VA Hospitals Attract Bad Physicians?
USA Today’s investigation found substantial evidence to suggest that Schneider’s case isn’t an isolated event. In fact, Donovan Slack’s story paints a picture of a federal agency, established to protect and promote veteran health, that actually attracts the worst doctors in the country.
A psychologist was hired in Louisiana despite his history of felony convictions. In Oklahoma, a psychiatrist who had already been penalized for sexual improprieties went on to sleep with one of his patients at a VA hospital. Scouring case after case, Slack and colleague Michael Sallah began to gain an impression of a Veterans Affairs office that protected bad physicians, rather than punishing them.
VA policy is probably exacerbating the problem. Doctors who work for the Department of Veterans Affairs don’t need malpractice insurance; negligence settlements are paid out by the federal agency using taxpayer dollars. That could make the VA a safe harbor for physicians with past records of misconduct and poor care, who are too risky for private insurers to cover.
Doctors Allowed To Resign, Continue Working
In total, the USA Today investigation uncovered around 230 secret medical malpractice settlements paid out by the US Department of Veterans Affairs, records that had never before been released for public scrutiny. Over 100 VA facilities in 42 different States were implicated.
Some of the settlements pertain to whistleblower cases, in which employees who accused the federal agency of wrongdoing were apparently silenced with cash payments. In other cases, “it’s clear the employees were the problem,” Slack and Sallah write.
In 126 of the cases, VA investigations deemed the misdeeds of government doctors so severe that it recommended firing the physicians. And in 70 of the settlements, the problem doctors were banned from working in VA hospitals. But instead of warning other medical providers, the VA often chose to keep quiet about the malpractice. “In nearly three-quarters of [the] settlements,” USA Today reports, “the VA agreed to purge negative records from personnel files or give neutral or positive references to prospective employers.”
New VA Leaders Hope To Clean Up Veterans Health Care
After USA Today’s story first broke in October 2017, officials at the Department of Veterans Affairs were quick to make changes. Current Secretary of Veterans Affairs, David J. Shulkin, M.D., says that all settlements with VA employees over $5,000 will now be sent for approval to the agency’s highest representatives in Washington, D.C. And individual cases, including the case of neurosurgeon John Henry Schneider, will now receive “independent third-party clinical review.”




Leave A Comment